There are no items in your cart
Add More
Add More
| Item Details | Price | ||
|---|---|---|---|
When we think about kidney health, we usually picture lab reports, blood pressure, hydration, or protein intake. But research is uncovering a fascinating connection between our digestive system and our kidneys—one that might just change how we prevent and manage kidney disease. It's called the gut-kidney axis.
This relationship between our gut microbes and kidney function is more than a curious biological insight—it's a game-changer. From managing inflammation to modulating blood pressure and slowing the progression of chronic kidney disease (CKD), the gut-kidney axis offers promising new directions in health, nutrition, and medicine.
Let’s break down what this axis is, why it matters, and how you can support it with smart dietary and lifestyle strategies.
What is the Gut-Kidney Axis?
The gut-kidney axis describes the two-way communication between the gut microbiome—the diverse community of bacteria, fungi, and other microbes in the gastrointestinal tract—and the kidneys.
When your kidneys aren’t functioning well, waste products like urea start to build up in the body. Some of that urea makes its way into the gut, where it can disrupt the balance of healthy bacteria. This leads to a condition known as gut dysbiosis.
In return, these harmful bacteria produce toxic byproducts like indoxyl sulfate and p-cresyl sulfate, which get absorbed into the bloodstream. If the kidneys are already struggling, they can’t efficiently remove these toxins—so they stick around and cause even more damage. This feedback loop fuels inflammation, oxidative stress, and accelerates kidney disease (Evenepoel et al., 2017; Chen et al., 2019).
The Trouble with Uremic Toxins
The gut microbiome plays a dual role. It can be a friend—producing anti-inflammatory compounds like short-chain fatty acids (SCFAs)—or a foe—releasing toxic substances if the wrong bacteria take over.
In CKD, dysbiosis often leads to an overproduction of:
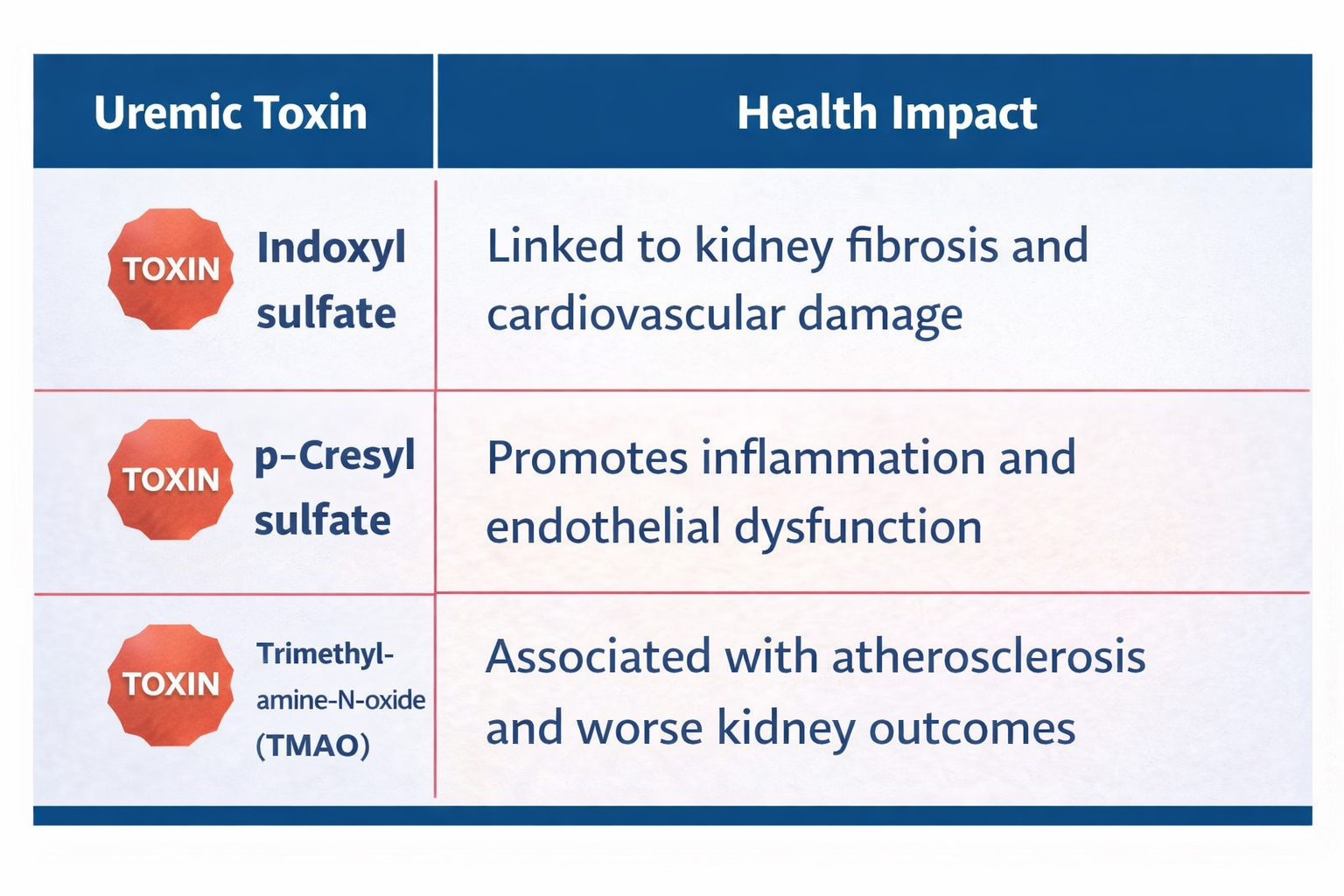
These toxins are known as uremic toxins, and unfortunately, even dialysis struggles to fully clear them. That’s why supporting gut health early is essential (Yang et al., 2018).
More Than Just Kidneys: The Brain-Gut-Kidney Triangle
Emerging studies point to a deeper connection between our brain, gut, and kidneys. This three-way axis plays a role in blood pressure regulation, mood, and cognition. People with CKD often experience depression, anxiety, and cognitive decline—and the gut may be part of the story. Poor gut health contributes to systemic inflammation and may even affect neurotransmitter production (Vallianou et al., 2023). So, supporting your gut could mean clearer thinking, better blood pressure control, and stronger kidneys.
Diet, Microbes, and the Gut-Kidney Axis
The good news? Diet is one of the most powerful tools for influencing your gut microbiome—and by extension, the health of your kidneys. Here’s what helps:
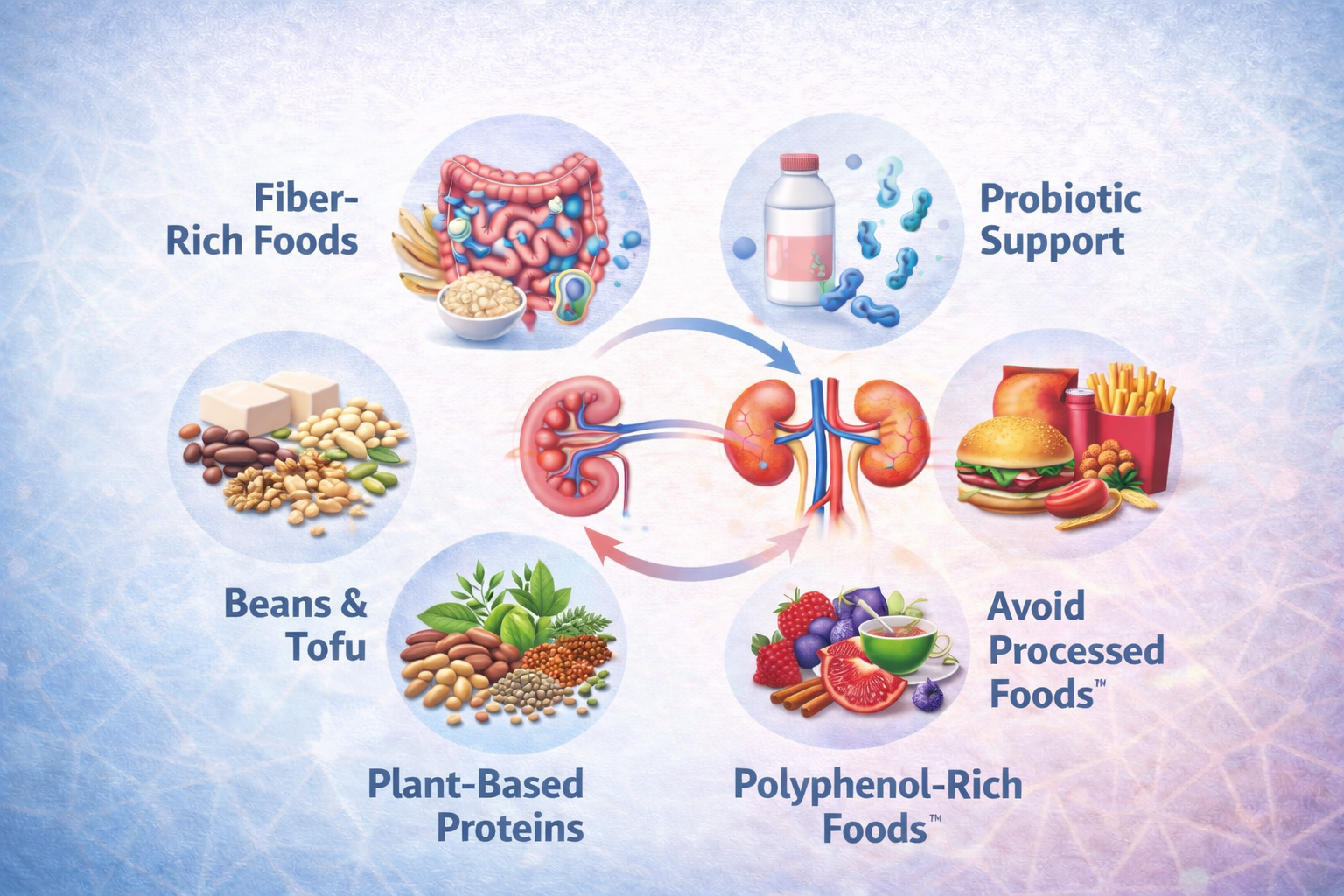
1. Fiber-Rich Foods Fibers found in foods like oats, lentils, bananas, and whole grains act as prebiotics, feeding beneficial gut bacteria.
Note: People with advanced kidney disease need to monitor potassium and phosphorus levels when increasing fiber.
2. Probiotic Support Probiotics are live beneficial bacteria that help restore balance in the gut. In people with kidney disease, certain strains (Lactobacillus, Bifidobacterium) may reduce levels of uremic toxins (Tsuji et al., 2024).
3. Plant-Based Proteins Swapping some animal protein for plant-based sources like beans and tofu can reduce TMAO formation.
4. Polyphenol-Rich Foods Berries, dark chocolate, green tea, and turmeric support a healthy microbiome and reduce inflammation.
5. Avoid Processed Foods Additives and preservatives can harm gut bacteria and stress the kidneys.
Why This Matters for Healthcare and Wellness
This gut-kidney connection has big implications:
Even for those without kidney disease, supporting gut health now could protect against renal issues later.
What we eat doesn’t just affect digestion—it shapes our internal ecosystem. The gut-kidney axis is part of a broader network that’s central to modern health science. Whether you're managing a chronic condition or simply aiming for better long-term health, your gut might be the best place to start.
Gut-Kidney Axis MasterclassWant to learn more Gut-Kidney Axis in Details? Join our quick Masterclass Gut-Kidney Axis . Click on the button above, enroll and start learning immediately
{{AUTHORS}}
Ms. Sara Sakarkute is a Master's student pursuing Nutrition and Dietetics with a focused interest in clinical nutrition and lifestyle-based interventions. She applies evidence-based nutrition principles to support preventive health, metabolic balance, and long-term well-being.
Ms. Mugdha Deshpande, RD, has submitted her PhD thesis in Health Sciences and has an advanced degree in nutrition and dietetics. She currently serves as a Research Scientist at Hirabai Cowasji Jehangir Medical Research Institute, Jehangir Hospital Pune.